Intradermal injection is a technique of administering medication into the dermis, the layer just below the epidermis of the skin. Vial preparation ensures that the correct dosage is withdrawn safely from a vial while maintaining aseptic technique. This procedure is often used for skin tests, such as tuberculosis or allergy testing, where a small amount of medication is injected to observe a localized reaction.
Why is this procedure performed?
- To safely prepare and administer intradermal medications
- To maintain aseptic technique and prevent contamination
- To ensure accurate dosage and effective medication delivery
- To observe for local reactions for diagnostic purposes
- To protect both patient and healthcare provider from infection or injury
Materials Needed
- Medication card
- Sterile gloves
- Medicine tray
- Black ink pen
- Prescribed medication in vial
- Sterile water bottle
- 1cc syringe
- Aspirating needle g.20 or g.18
- Cotton balls: Dry and Wet (70% Alcohol) in separate containers
Assessment
- Review the physician’s order and medication record for the medication to be given.
- Assess the site if the patient has had other intradermal injections.
- Assess the need for assistance.
Planning
- Determine materials needed.
- Wash your hands.
- Gather all materials needed.
Implementation
- Verify the right drug to be administered by:
- Reading the name of the medication from the record
- Checking the label on the medication before picking it up
- Checking the label again before calculating and preparing the dose
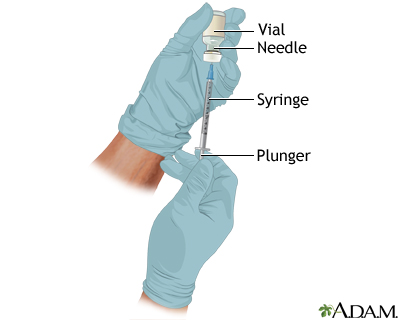
Vial Preparation
- Remove the metal or plastic cap on the vial that protects the rubber stopper.
- Swab the rubber top of the vial using cotton balls with alcohol.
- Remove the cap from the needle by pulling it straight off.
- Inject the amount of air equal to the volume of the medication you are going to withdraw, then remove the syringe.
- Pick up the vial with your non-dominant hand and hold it upside down at eye level, making sure the needle tip is below the fluid level. Pull the plunger down to draw the necessary amount of medication, then withdraw the syringe once the correct dose is obtained. For skin testing preparation, the ratio is 0.1ml medication to 0.9ml sterile water.
- If any air bubbles accumulate in the syringe, tap the barrel to move them to the top and push the plunger to expel the air.
- If a multi-dose vial is being used, label the vial with the date and time it is opened, and store the vial according to agency policy.
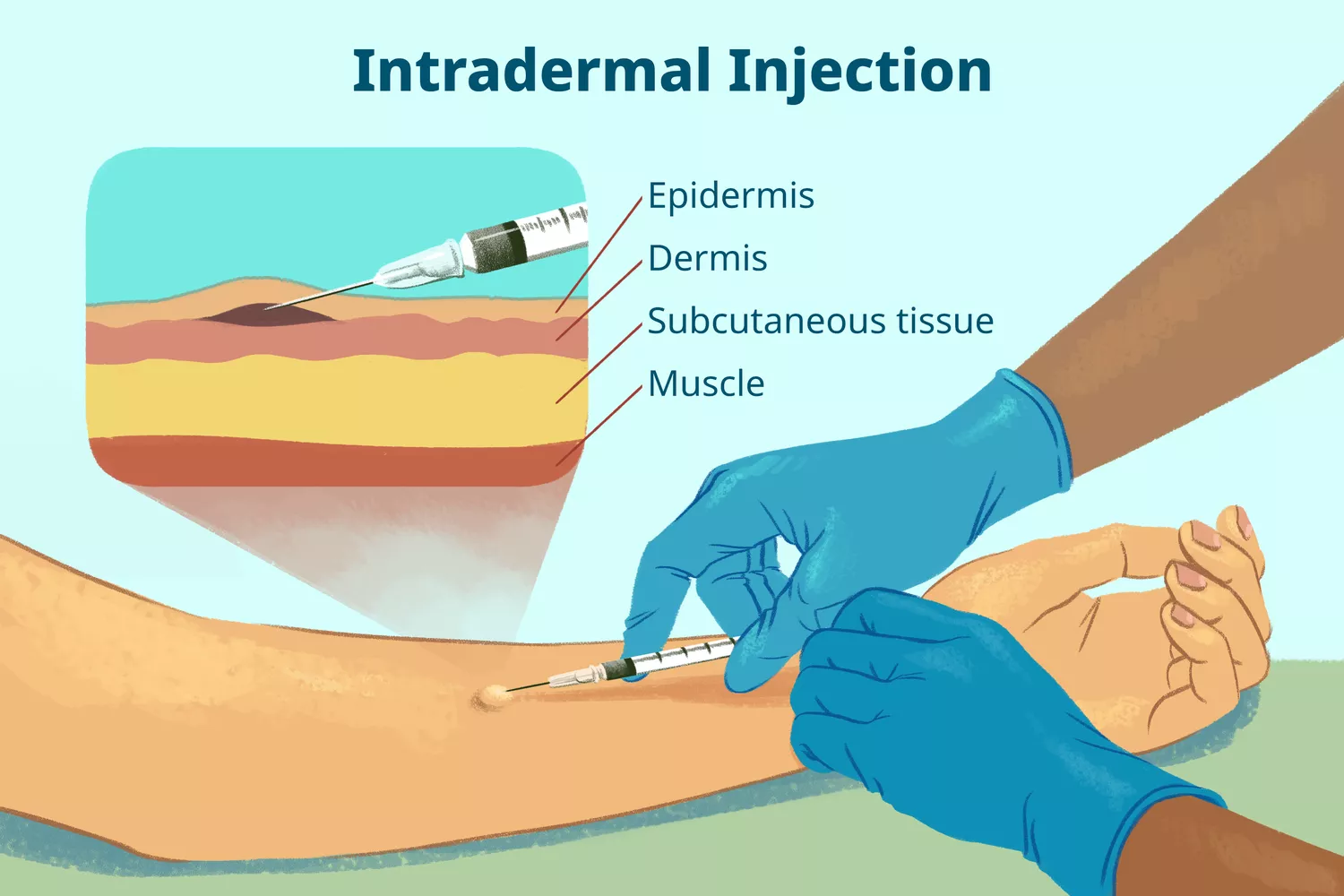
Intradermal Injection
- Don sterile gloves.
- Clean the area around the injection site with an alcohol swab in a firm, circular motion, moving outward, and allow the antiseptic to dry.
- Hold the syringe with your dominant hand between thumb and forefinger. Remove the needle cap with the non-dominant hand, pulling it straight off.
- Place a dry cotton ball between the fingers of your non-dominant hand.
- Pull the skin at the site taut using your non-dominant hand. For ventral forearm, place the hand on the dorsal forearm and pull to tighten ventral skin.
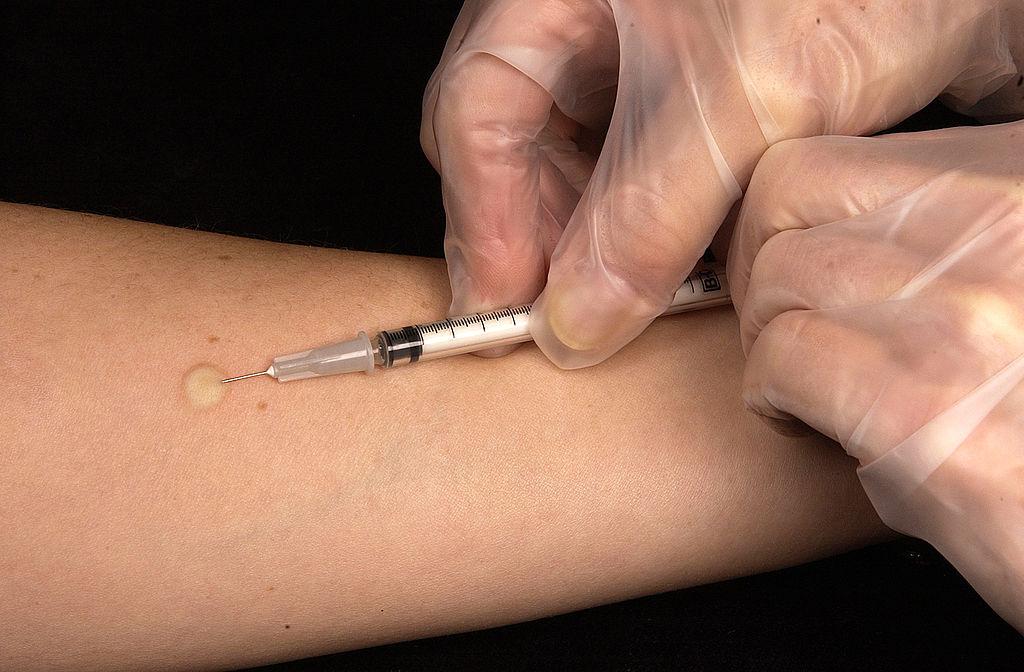
- Stabilize your hand and inject the needle bevel up at an angle of 10º–15º, parallel to the skin, ensuring the entire lumen is in the dermis.
- Slowly inject the medication while watching for a small wheal or blister to appear.
- Withdraw the needle at the same angle and wipe excess medication with the cotton ball. Never massage the area.
- Encircle the site directly over the borders with a black marking pen and assess the site for reaction at the appropriate time (30 minutes after administering medication).
- Do not recap the used needle. Discard the needle and syringe in the appropriate receptacle.
- Remove gloves and dispose of them properly.
- Assist the client to a position of comfort.
- Wash your hands.
Evaluation
Evaluate using the following criteria:
- 10 rights followed
- Correct site used
- Effectiveness of medication assessed
- Any side effect promptly identified
Documentation
Record pertinent data in terms of:
- Medication dosage
- Route of administration
- Time of administration
- Signature